From furthering our basic understanding of infectious organisms, such as bacteria, viruses, fungi and parasites (collectively known as pathogens), all the way to creating new treatments and even cures, animal research has been, and continues to be, a major contributor in our fight against infectious diseases, both to protect the health of humans and animals too. For now, information from animal studies is crucial for the discovery of entirely new treatments and the development of improved ones that have a widespread effect and benefit.
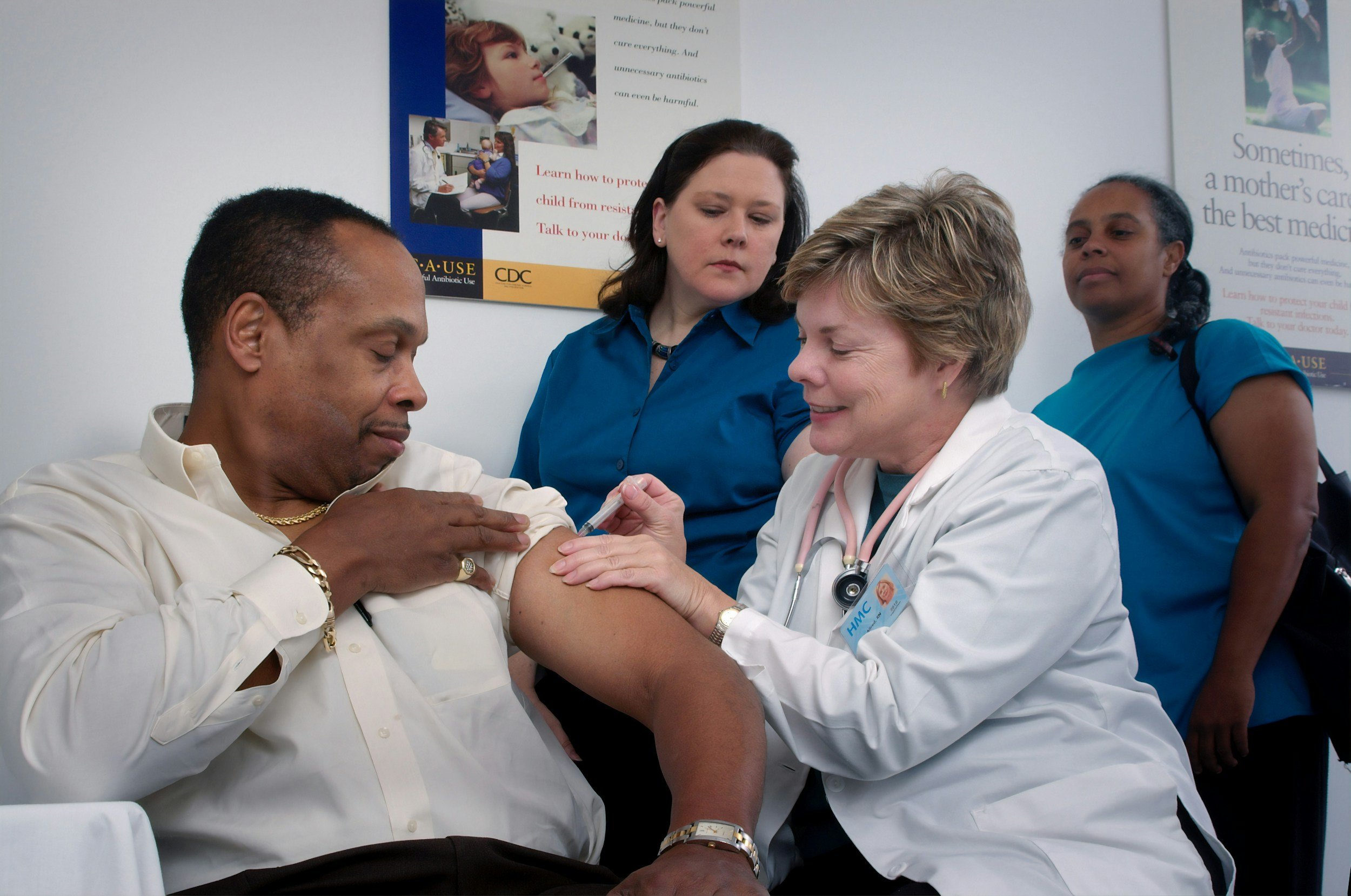
Why are animals used in infectious disease research?
An animal model can be useful to, in a very short time sometimes, show proof of concept – of how the virus transmits, or how it causes disease – but also if you want to test interventions. It is difficult to test interventions that are focused on preventing infection in humans.
Koen van Rompay, California National Primate Research Center, USA
Using animals in Covid-19 research
If the animal trials showed the vaccine was not safe, or not effective, we would not have wasted time preparing clinical trials that could not go ahead. This time, we did all the clinical trial preparation while the animal trials were still going on.
That way, it was within days of receiving the safety data from our animal trials that we were putting the vaccine into the arms of our first volunteers.
Professor Dame Sarah Gilbert, Oxford Vaccine Group, UK
Which research on infectious diseases benefits from animal research?
A universal vaccine targeting a range of strains of meningitis B, which affects the brain, has been developed by EARA member Novartis, Switzerland, which used earlier research in mice and rats. Novartis researchers were able to create the vaccine by searching the genome of the Neisseria meningitides bacterium (the main cause of meningitis) for proteins that could be targeted by antibodies, before producing these antibodies in mice and testing whether they could kill the bacteria. Rats treated with the mouse antibodies confirmed that the vaccine worked and could be rolled out to protect thousands from disability and death.
Zebrafish have also been used to study meningitis. A study at the Paris Brain Institute, France, and UMC Amsterdam, Netherlands, identified that brain neurons that detect bitter tastes played a role in protecting against bacterial meningitis.
Chronic myeloid leukaemia (CML) is one such rare cancer that develops slowly over a person’s lifetime, but thanks to medical advances can now be kept under control with the right treatments. Studies in mice were an instrumental part in finding the protein abnormality that causes CML. The precision medicine Gleevec was developed, by Oregon Health & Science University, USA, to just target this protein abnormality in cancer cells in mice (not targeting all cells, like most chemotherapy drugs), and was later used to reduce cancer growth in CML patients. Other species, including dogs, rabbits and monkeys, were also involved in the development of Gleevec (and its rapid approval by the US Food and Drug Administration), by shedding light on how the drug behaved in the body and potential toxicities.
There are several different types of rare cancer that start in childhood, including neuroblastoma that mainly affects children under five-years-old and starts in nerve cells called a neuroblast, often in the adrenal glands located on the top of each kidney. Several studies in mice have contributed to improving survival rates and developing treatments with less severe side effects, for example a team at the University of Gothenburg, Sweden, were able to find an effective drug that worked against one of the two gene mutations that cause neuroblastoma.
Mice were also used in a study of the rare eye cancer retinoblastoma (which mainly affects young children) at the St Jude’s Research Hospital, USA, to confirm that the cancer’s cause was not a series of mutations, like most cancers, but the loss of a single gene – explaining why it develops so quickly.
An animal model can be useful to, in a very short time sometimes, show proof of concept – of how the virus transmits, or how it causes disease – but also if you want to test interventions. It is difficult to test interventions that are focused on preventing infection in humans.
Koen van Rompay, California National Primate Research Center, USA
What is antibiotic resistance?
However, in recent years, with the over-frequent use of antibiotics for both humans and animals, a phenomenon in bacteria known as antibiotic resistance is becoming a major global health threat. This has already rendered many drugs ineffective and is only set to get worse. Ultimately completely new ways will be needed to treat bacterial infections.
Animal studies will be essential for testing alternatives to antibiotics. Phage therapy, which uses viruses to infect and kill bacteria, is emerging as a promising alternative to antibiotics, but before it can be trialled in humans, animals have been essential to testing, refining and improving this approach so it can be used in the clinic.
Species ranging from mice to rabbits to chickens have been used to investigate phage therapy in a range of organ systems (such as the gastrointestinal) and bacterial strains. As farm animals like cows and pigs are given many antibiotics (even when they may be healthy), they are of particular interest in the study of antibiotic resistance, where diseases such as bovine tuberculosis and avian or swine flu are prevalent and pose a major health and economic burden.
Researchers at EARA members University Libre des Bruxelles and GSK, Belgium, have also looked into making existing antibiotics effective again, using mice to show that a molecule could reverse resistance against tuberculosis bacteria.
A lot of stuff can be done in Petri dishes, but then when it comes to testing the efficacy and potency of antibiotics, one has to look at animals models.
Professor Gad Frankel, Imperial College London, UK
Which animals are used in infectious diseases research?
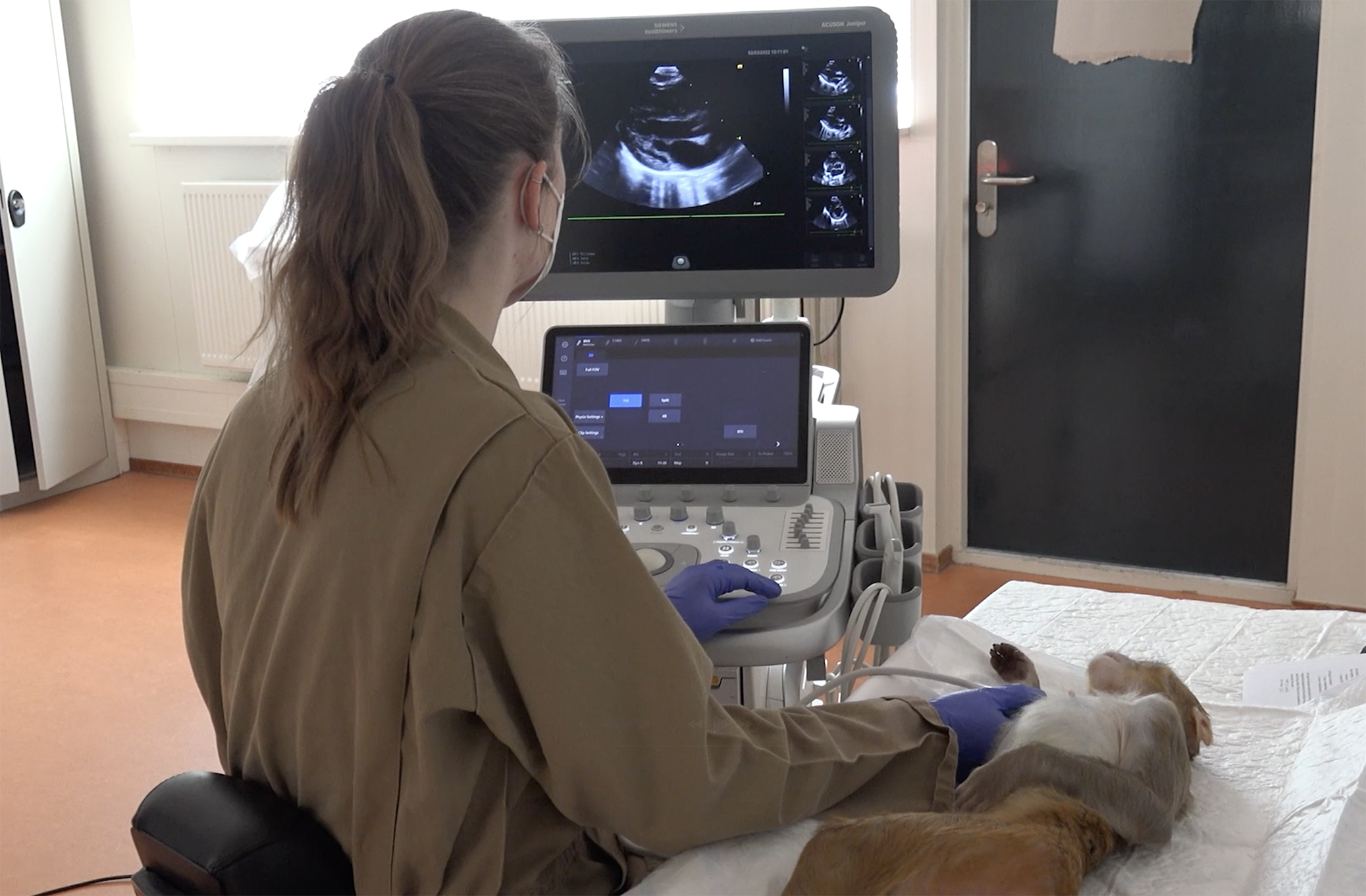
Infectious disease research benefits from studying a range of other animals, such as ferrets and guinea pigs which naturally catch strains of human flu, for example, and therefore display similar symptoms.
Meanwhile, the embryos of chickens develop in a way that is comparable to human foetuses and are therefore useful for studying early infection in diseases like Zika.
More unconventional species such as insects – from moths to mosquitos to honeybees – are also emerging as valuable models, since they can be easily manipulated, for example at the genetic level, to help understand the factors that contribute to infection mechanisms, disease progression and much more. Insects have additional value because certain pathogens (such as the plasmodium parasite for malaria) use insects as a host to infect other organisms, and can also be used to better understand antibiotic resistance.
While pigs do not naturally get cystic fibrosis (CF) they can be bred to develop very similar symptoms to the condition, such as lung disease which can naturally develop as a result – the lungs of pigs have been shown to be affected in a very similar way to those of humans. This means that interventions can be tested at an earlier stage than in a patient, in turn allowing researchers to come up with measures that could help to ease symptoms or detect the condition earlier on.
Pigs have also been geneticalms to people with the condition compared to rodents, such as difficulties with walking and running with age. In addition, certain brain changes were similar, such as the loss of specific neurons and immune responses.
Meanwhile, the same similarities in body make-up to humans have also meant that pigs have been used to model Huntington’s disease, a rare disorder where the brain’s nerve cells are damaged, and that can affect movement, behaviour and communication, among other effects.
In a study from Emory University, USA, and Jinan University, China, the genome of pigs was edited using CRISPR to insert the human gene that causes Huntington’s. This approach resulted in pigs that showed very similar symptoms to people with the condition compared to rodents, such as difficulties with walking and running with age. In addition, certain brain changes were similar, such as the loss of specific neurons and immune responses.
Limitations of animal models
How are animals cared for?
In the case of animal welfare, an improved range of aspects are important to maximise the well-being of animals, and the accuracy and reliability of experiments, from good experimental design to housing enrichment to harm-benefit analysis (whether the harms that animals are expected to experience justify the benefits of the research).
